5-day Advanced Vestibular Accreditation Pathway
Advanced Neuro Education is pleased to announce the launch of our new Advanced Vestibular Accreditation pathway, commencing in Q2 2026.

To achieve Advanced Vestibular Accreditation, participants complete two components:
2 days Accredited Practical Assessment & Management of the Dizzy Patient
(Face to face)
+
3 days Accredited Advanced Vestibular Modules
(Flexible online)
About Associate Professor James McLoughlin
Associate Professor James McLoughlin is a clinical academic Neurological and Vestibular Physiotherapist with over 25 years of experience in vestibular rehabilitation across private practice, elite sport, and neurological populations.
His academic and research career spans internationally recognised institutions including Queen Square, University College London, UNSW Sydney, Neuroscience Research Australia, and Flinders University. His work has contributed to the understanding of vestibular function, balance, and movement control, with over 30 peer-reviewed publications across diverse clinical populations.
Since 2007, James has delivered his flagship 2-day practical dizziness course globally, training physiotherapists and health professionals across Australia, the UK, and beyond. This course—and the broader 5-day Advanced Vestibular Accreditation pathway—has continuously evolved to reflect the latest evidence, emerging technologies, and real-world clinical insights.
What differentiates this pathway is its strong emphasis on clinical reasoning, treatment application, and implementation. While foundational vestibular science, diagnostic frameworks, and key clinical trials are covered, the primary focus is on translating knowledge into everyday practice. James is a firm believer that this knowledge base can and should be usable and accessible to all physiotherapists.
Participants develop the confidence and capability to:
- Apply vestibular principles across complex and chronic presentations
- Integrate vestibular assessment and treatment into musculoskeletal, sports, neurological, and geriatric rehabilitation
- Enhance patient outcomes through structured, evidence-informed clinical reasoning
- Implement practical models of care within their own clinical settings
This is not just a course—it is an enjoyable structured pathway designed to elevate clinical practice, expand professional scope, and support physiotherapists in delivering high-value, contemporary care across a wide range of patient populations.

2 days Accredited Practical Assessment & Management of the Dizzy Patient
(Face to face)
This intensive practical course focuses on:
Clinical assessment of the dizzy patient
Differential diagnosis of common and complex vestibular presentations
Bedside vestibular testing
Evidence-based management strategies
Over 10 common BPPV canal repositioning manoeuvres + atypical presentations
Integration of vestibular, visual and cervical systems
This course forms the practical foundation of the 5-day accreditation pathway.
Contact us to organise this practical course in your region or workplace.
Advanced Vestibular Rehabilitation Modules
Advanced Practice in Vestibular Rehabilitation extends beyond foundational skills, equipping clinicians with the expertise to manage complex and diverse presentations with confidence.
This program covers chronic and atypical vestibular conditions, paediatric populations, neurological disorders, and concussion. It integrates functional neuroanatomy, interpretation of clinical investigations, and the application of validated outcome measures to elevate clinical reasoning and treatment precision.
Delivered through 8 advanced online modules, the course allows you to learn at your own pace.
Completion of all modules, alongside our established 2-day face-to-face course, leads to Advanced Vestibular Accreditation Certification through Advanced Neuro Education.
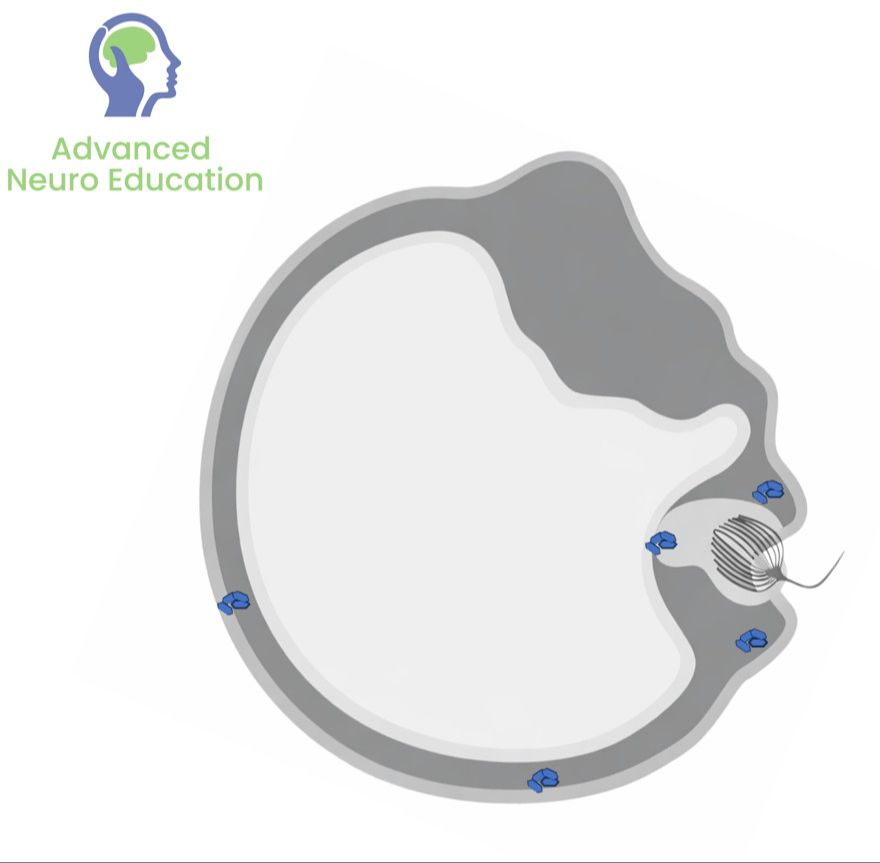
Complex and Atypical BPPV
By the end of this module participants will be able to;
- Differentiate Complex Variants: Distinguish between typical canalithiasis and complex variants such as Anterior Canal BPPV, Heavy/Light Cupula, and Canal Jams based on nystagmus characteristics.
- Analyse Anatomical Subtypes: Identify short-arm (ampullary) versus long-arm (non-ampullary) canalithiasis in both Horizontal and Posterior canals and explain their impact on nystagmus direction (geotropic vs apogeotropic).
- Diagnose "Invisible" BPPV: Recognize Type 2 BPPV and "Sitting-up Vertigo" as distinct entities characterized by symptoms and truncal oscillation often without typical paroxysmal nystagmus during provocation.
- Master Advanced Lateralization: Apply advanced diagnostic protocols (Null Points, Bow and Lean, pseudo-spontaneous nystagmus) to lateralize Light Cupula and apogeotropic HC-BPPV when the Supine Roll Test is inconclusive.
- Apply Advanced Maneuvers: Select and execute appropriate maneuvers for specific variants, including the Short CRP for AC-BPPV, the Zuma maneuver for HC-BPPV, and the Shigeno correction to prevent postural crises.
- Evaluate Recurrence: Understand the random nature of BPPV recurrence patterns and the limitations of predicting future affected canals based on prior episodes.
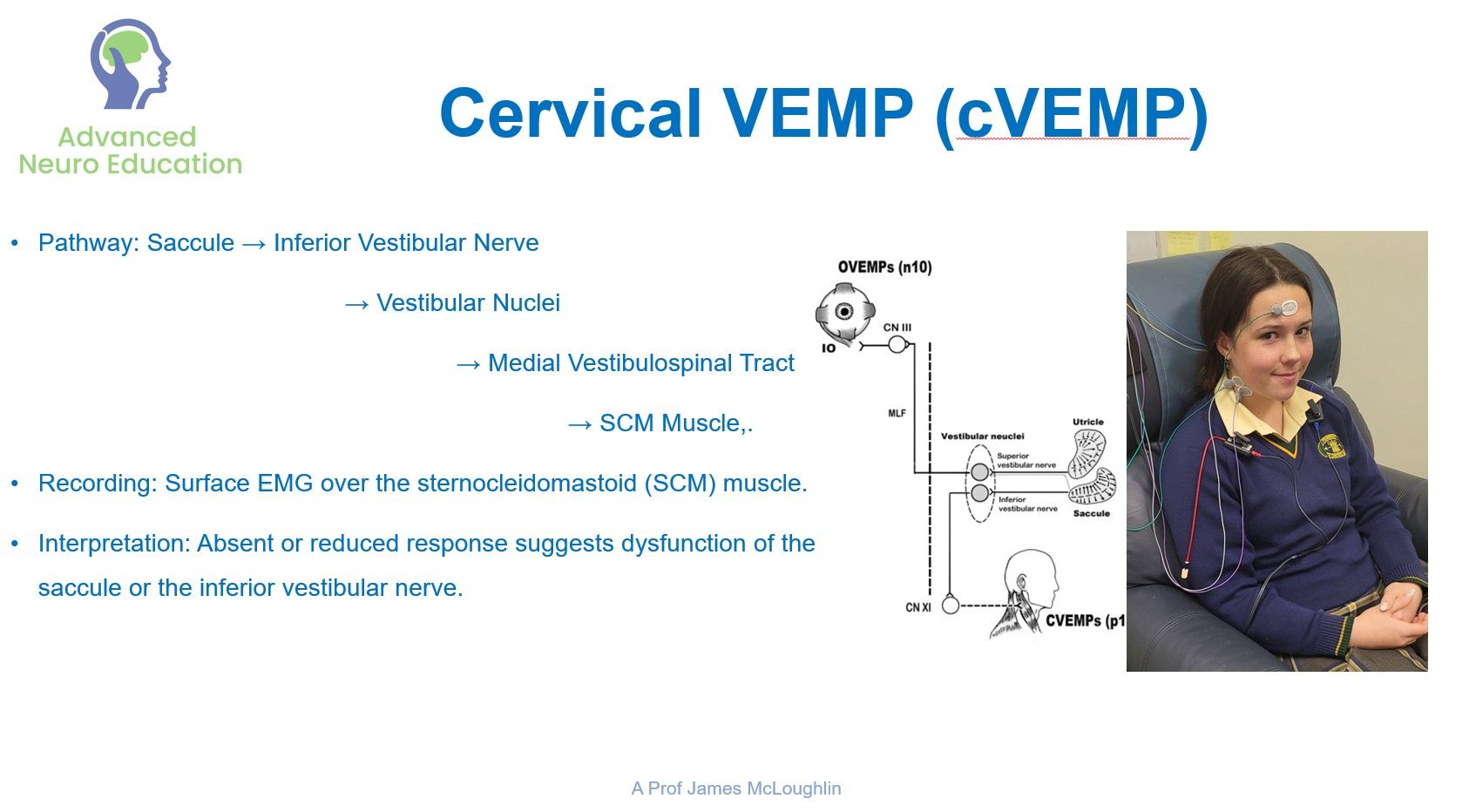
Vestibular investigations and technology
By the end of this module participants will be able to;
- Differentiate and Interpret Vestibular Laboratory Tests: Critically analyze the anatomical targets and clinical utility of Video Head Impulse Testing (vHIT), Caloric testing, and Vestibular Evoked Myogenic Potentials (cVEMP and oVEMP) in diagnosing peripheral vestibular hypofunction. Have some awareness of Rotatory Chair Testing.
- Apply Common Outcome Measures: Select and interpret standardized vestibular outcome measures, specifically the Dizziness Handicap Inventory (DHI) and Dynamic Visual Acuity (DVA), to quantify disability and monitor rehabilitation progress,.
- Analyze Oculomotor and Eye Tracking Dysfunction: Utilize advanced eye-tracking parameters (e.g., anti-saccades, smooth pursuit) to differentiate central from peripheral pathologies using technologies like VNG and NeuroFlex,.
- Implement Advanced Diagnostic Algorithms: Apply evidence-based bedside algorithms (HINTS, STANDING) and evaluate skew deviation to rule out central pathologies like stroke in acute vestibular syndrome,,.
- Evaluate Virtual Reality Applications: Critically appraise the efficacy of Virtual Reality (VR) and Augmented Reality (AR) in vestibular rehabilitation, fall prevention in the elderly, and performance analysis in sports.
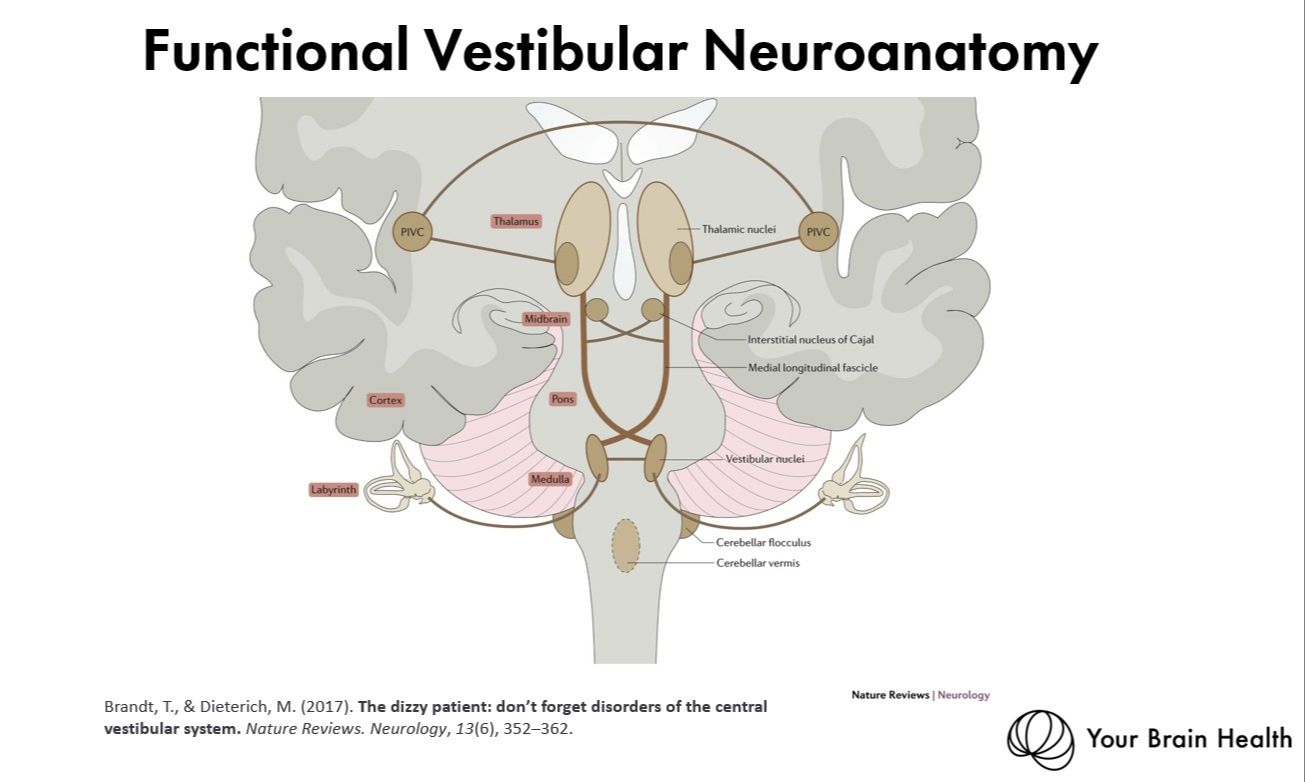
Vestibular Functional Neuroanatomy
By the end of this module participants will be able to;
- Anatomically Differentiate: Distinguish the functional contributions of the otolith organs (utricle/saccule) versus semicircular canals and their specific projections to the vestibular nuclear complex.
- Map Neural Pathways: Trace the ascending and descending pathways (vestibulospinal, reticulospinal, corticospinal) and their roles in maintaining vertical support, postural tone, and rapid reflex modulation,.
- Analyze Oculomotor Control: Evaluate the neuroanatomy of the vestibulo-ocular reflex (VOR), saccades, and smooth pursuit to localize lesions within the brainstem (e.g., medial longitudinal fasciculus, interstitial nucleus of Cajal) and cerebellum.
- Interpret Cortical Processing: Critically assess the "vestibular neuromatrix," identifying the functional roles of the Parieto-Insular Vestibular Cortex (PIVC), area OP2+, and their connectivity to cognitive-affective regions (cingulate, insula, amygdala).
- Apply Advanced Diagnostics: Correlate clinical findings (e.g., HINTS+, nystagmus characteristics, visual dependence) with specific neuroanatomical substrates in stroke, concussion, and "Pusher syndrome",,.
- Evaluate Research Methodologies: Differentiate the utility and limitations of fMRI, Galvanic Vestibular Stimulation (GVS), and Caloric irrigation in mapping cortical vestibular networks and diagnosing central vestibular disorders.

Chronic vestibular conditions and PPPD
By the end of this module participants will be able to;
- Critically evaluate the multifactorial pathophysiology of chronic dizziness, particularly in the elderly, distinguishing between presbystasis and specific vestibular pathologies.
- Analyze the concept of visual dependence (visual vertigo) as a maladaptive sensory reweighting strategy and its impact on postural control and falls risk.
- Apply the Bárány Society diagnostic criteria to differentiate Persistent Postural-Perceptual Dizziness (PPPD) from structural vestibular disorders and psychiatric conditions.
- Formulate evidence-based multimodal management plans for PPPD, integrating vestibular rehabilitation, cognitive-behavioral therapy, and pharmacotherapy.
- Distinguish the overlapping clinical features of Vestibular Migraine, Meniere’s and Mal de Debarquement Syndrome (MdDS), specifically regarding symptom triggers and response to passive motion.
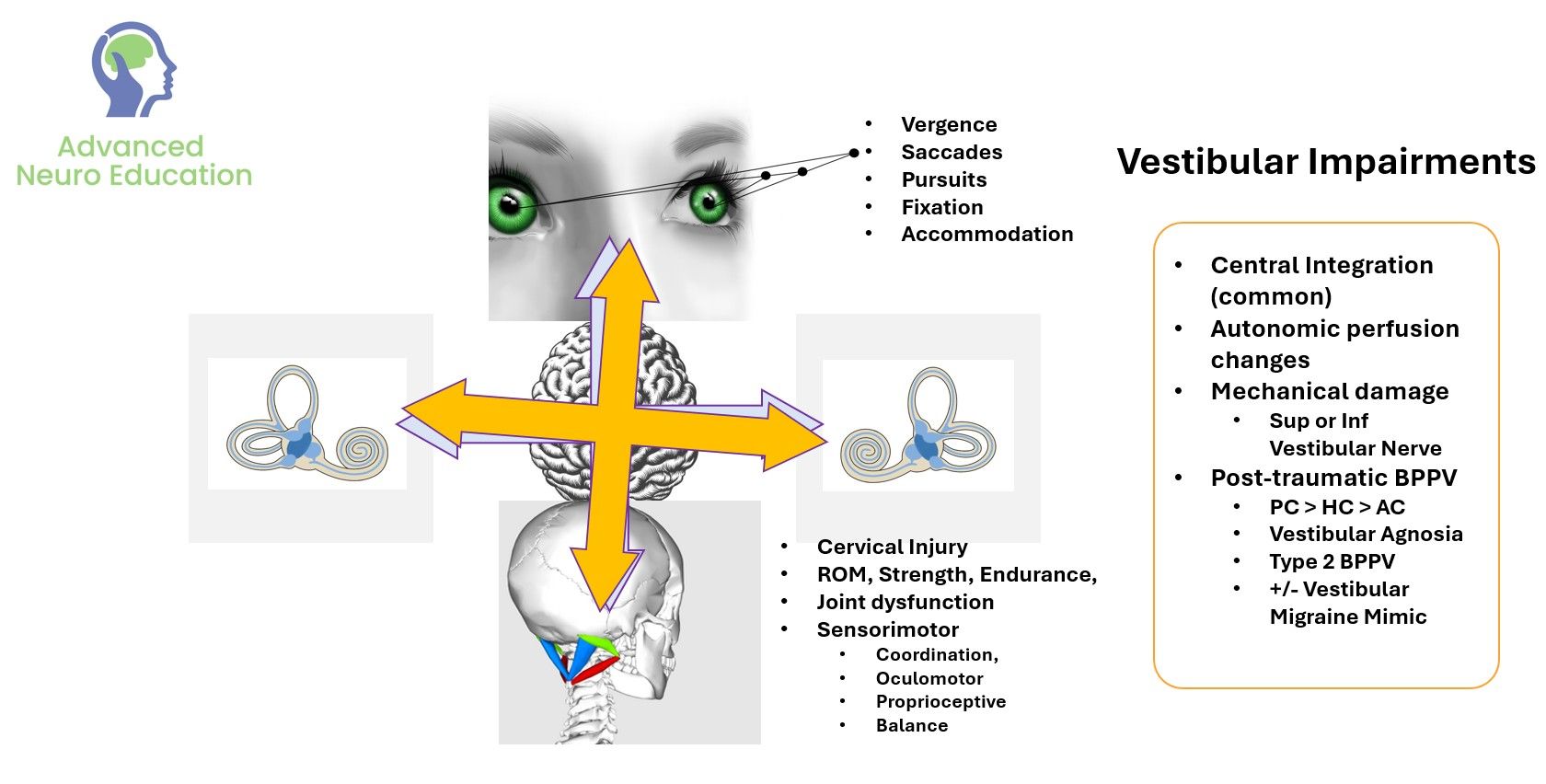
Concussion and vestibular rehabilitation
By the end of this module participants will be able to;
- Deconstruct the "Discombobulated State": Differentiate between the transient, physiological state of neural desynchronization (sensory mismatch, metabolic crisis) and permanent vestibular or neurological injury in the acute post-concussion phase.
- Evaluate Post-Traumatic BPPV: Identify the unique clinical features of post-traumatic BPPV, including vestibular agnosia, multi-canal involvement, and higher recurrence rates compared to idiopathic BPPV.
- Localize Vestibular Nerve Pathology: Analyze the specific vulnerability of the inferior vestibular nerve in persistent post-concussive symptoms (PPCS) using vHIT and cVEMP data, contrasting this with central cerebellar causes.
- Differentiate Cervicogenic Mechanisms: Assess cervical spine proprioception using Head Repositioning Accuracy (HRA) and Joint Position Error (JPE) testing to distinguish cervicogenic dizziness/Whiplash Associated Disorder (WAD) from labyrinthine dysfunction.
- Apply Multimodal Management: Synthesize evidence supporting early initiation of subthreshold aerobic exercise and targeted cervico-vestibular rehabilitation to address dysautonomia and sensorimotor deficits.
Vestibular Outcome measures
By the end of this module participants will be able to;
- Select and Administer Patient-Reported Outcome Measures (PROMs): Differentiate between measures of handicap (DHI), balance confidence (ABC, FES-I), and functional impairment (VADL) to capture the patient's subjective experience of dizziness and disequilibrium.
- Evaluate Static and Dynamic Balance: Competently apply and score functional tests including the Berg Balance Scale (BBS), BESS, TUG, and mCTSIB to assess steady-state and sensory integration balance deficits.
- Assess Gait under Vestibular Challenge: Utilize the Dynamic Gait Index (8-item and 4-item) to evaluate gait stability during head turns and speed changes.
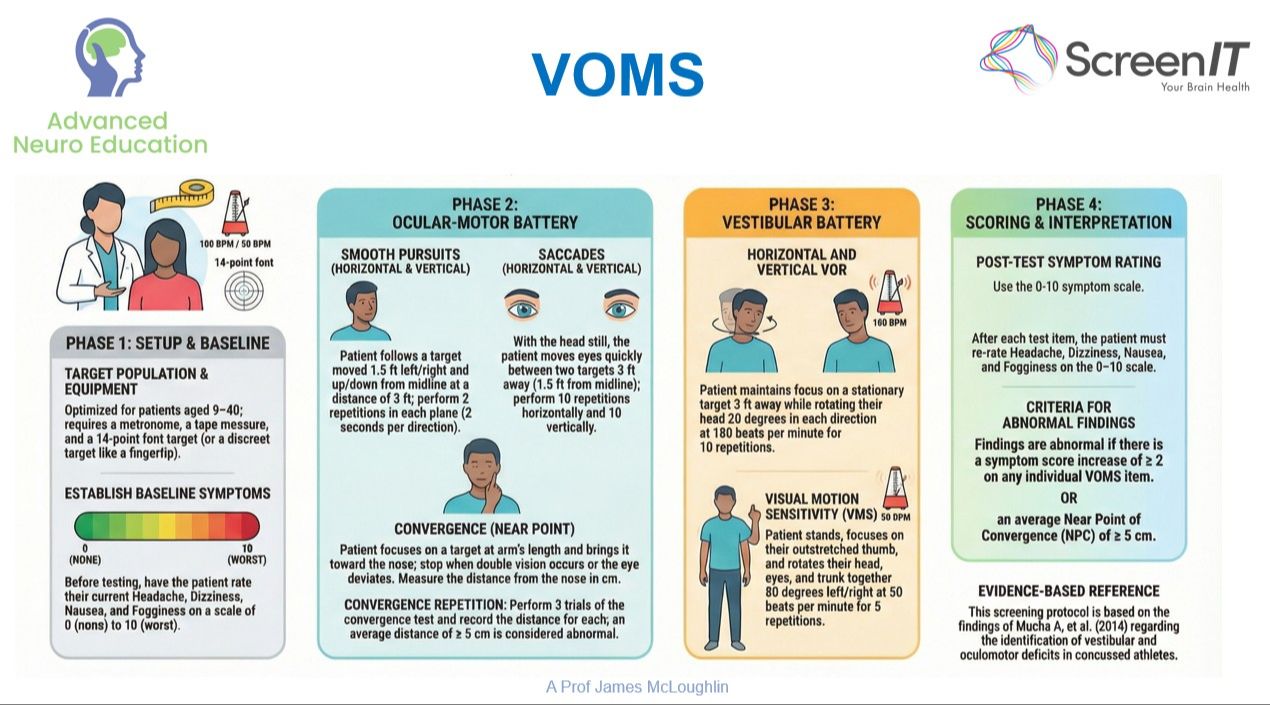
- Screen for Physiological Vestibular and Cervical Deficits: Interpret bedside tests such as HIT/vHIT, Dynamic Visual Acuity, VOMS, and Cervical JPE to differentiate between peripheral vestibular, central, and cervicogenic causes of dizziness.
- Quantify Motion Sensitivity, Vigilance and Psychosocial Impact: Use the MSQ to measure motion-provoked symptoms, Balance Vigilance Questionnaire (Balance- VQ) and screen for anxiety/depression (GAD-7, PHQ-9) as comorbidities in vestibular disorders.
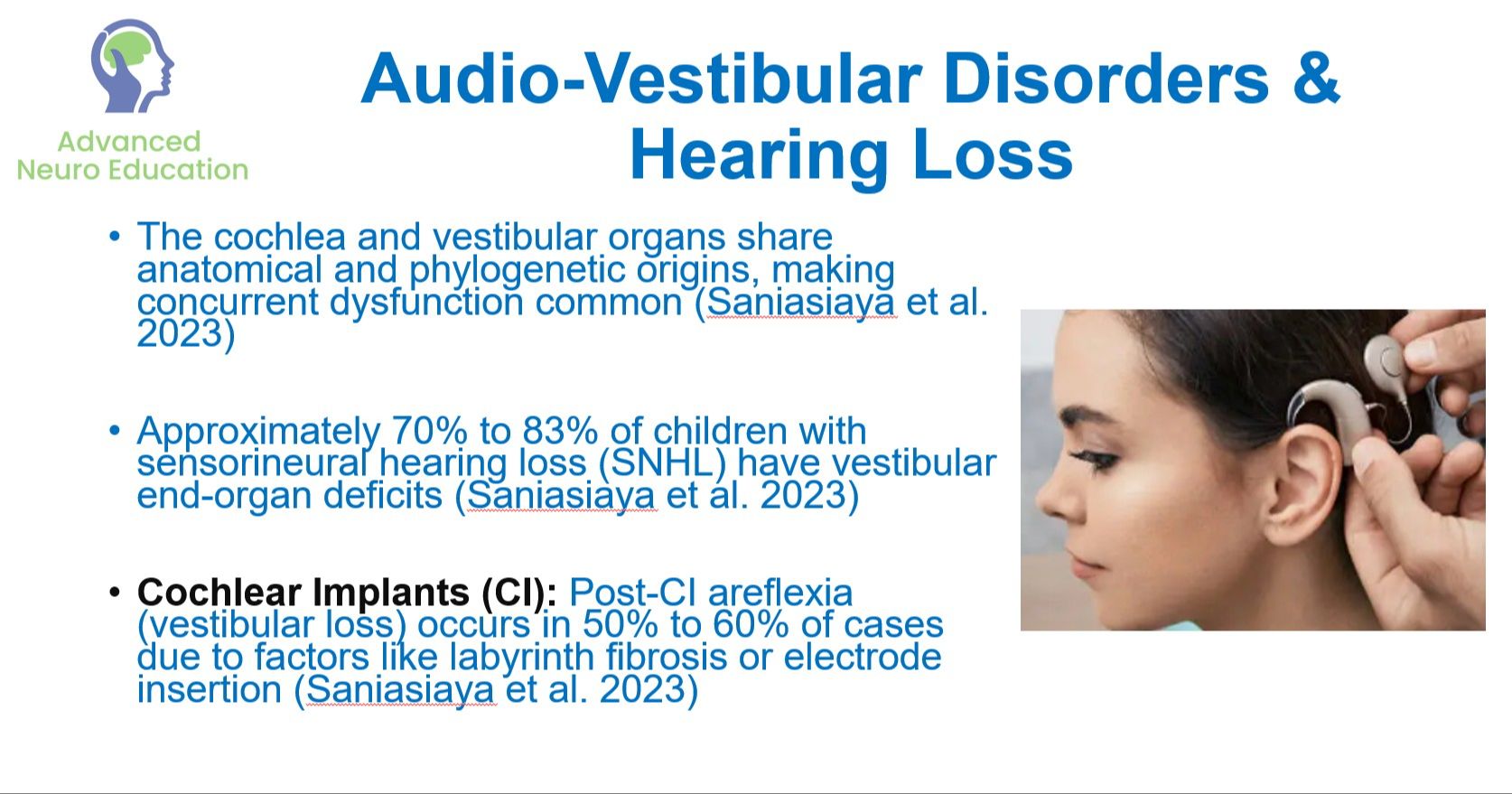
Paediatric Vestibular Assessment and Rehabilitation
By the end of this presentation, participants will be able to:
- Differentiate the clinical presentation of vestibular dysfunction in children compared to adults, including the varied expression of symptoms and the impact on developmental milestones.
- Identify the most common vestibular conditions specific to the paediatric and adolescent populations, such as Vestibular Migraine, Benign Paroxysmal Vertigo of Childhood (BPVC), and audio-vestibular disorders.
- Recognize the unique challenges of paediatric vestibular assessment and the necessity of objective, age-appropriate testing.
- Apply developmental principles to paediatric vestibular rehabilitation (VR), specifically understanding the concept of critical periods and why substitution strategies differ significantly between children and adults.
- Design effective, age-appropriate vestibular rehabilitation exercises that utilize play-based therapy to maximize patient engagement and motor learning.

Vestibular Rehabilitation and Neurological Disorders
By the end of this module participants will be able to;
- Analyse the Core Elements of Vestibular Rehabilitation (VR): Deconstruct the mechanisms of restoration, habituation, and adaptation, and apply specific interventions such as Canalith Repositioning Treatments (CRTs) for BPPV, gaze stability exercises, and dynamic balance training.
- Evaluate the Vestibular-Cognitive Link: Explain the physiological connection between the vestibular system, the hippocampus, and spatial awareness, and identify how vestibular deficits contribute to spatial disorientation and cognitive decline.
- Assess Fall Risk Mechanisms: Correlate vestibular dysfunction with postural instability and fall risk across various neurological pathologies, distinguishing between peripheral and central causes.
- Apply VR Strategies to Specific Neurological Conditions:
◦ Multiple Sclerosis: Integrate findings on the efficacy of VR for reducing fatigue and improving balance.
◦ Traumatic Brain Injury (TBI): Identify common vestibular sequelae like BPPV and gait ataxia in acute and chronic TBI.
◦ Stroke & Parkinson’s: Formulate VR protocols to improve gait, posture, and oculomotor function.
◦ Alzheimer’s Disease: Recognize vestibular impairment as a potential biomarker and contributor to the "spatial" subtype of AD.
Contact us to arrange the
2 days Accredited Practical Assessment & Management of the Dizzy Patient (Face to face)
in your region.

